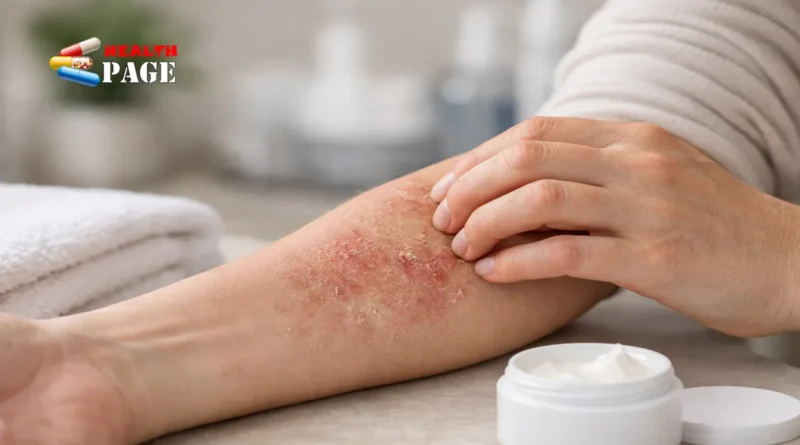
7 Powerful Facts on How Does Eczema Develop and Harm Skin Health
If you have ever wondered how does eczema develop, you are not alone. Many people blame dry weather, stress, or a new soap. Those triggers matter, but eczema usually starts deeper. It develops through a mix of genetics, immune system changes, and outside irritants that weaken the skin barrier over time. The result is skin that loses moisture fast, becomes inflamed easily, and falls into repeated flare-ups.
Eczema, also called atopic dermatitis, is more than simple dryness. It can itch intensely, disrupt sleep, affect confidence, and raise the risk of infection. For some, it begins in infancy. For others, it appears later in life without warning. Understanding the process helps people manage symptoms earlier and more effectively.
This article breaks down seven clear facts about eczema development, how it harms skin health, and what current research says in 2025–2026.
1. Eczema Is a Chronic Inflammatory Skin Condition, Not Just Dry Skin
When asking how does eczema develop, it helps to start with what eczema is. Eczema is a chronic inflammatory condition. That means the skin is not only dry, but also irritated by an ongoing immune response.
Common symptoms include:
- Dry, rough skin
- Itching that can become severe
- Red or darker inflamed patches
- Cracking or oozing skin
- Thickened skin after repeated scratching
Eczema often moves in cycles. A flare may settle, then return weeks later. This pattern makes it feel unpredictable.
Why this matters for skin health
Healthy skin acts like a wall. It keeps moisture in and irritants out. In eczema, that wall becomes weak. Water escapes, and allergens or harsh substances enter more easily. The skin then becomes more reactive, creating a repeating loop of dryness and inflammation.
A simple example is a child who scratches at night until the skin breaks. By morning, the area feels raw and stings with even mild lotion. That is not “just dry skin.” It is a damaged barrier under immune stress.
2. Genetics Often Set the Stage Before Symptoms Ever Appear
One of the strongest answers to how does eczema develop is genetics. Many people with eczema are born with a higher risk because of inherited changes in the skin barrier or immune system.
A key gene linked to eczema is the filaggrin (FLG) gene. Filaggrin helps the skin stay strong and hold moisture. When this gene does not work well, the skin barrier becomes leaky.
Genetic factors linked to eczema
- FLG mutations reduce barrier proteins
- Changes in tight junction genes weaken skin structure
- Some gene variants affect immune control
- Family history raises risk, especially with asthma or hay fever
This is why eczema often runs in families. A parent may have asthma, a sibling may have allergies, and a child may develop eczema. These conditions are part of what doctors call the “atopic march.”
Real-life example
An infant may develop eczema on the cheeks at three months old. Later, that same child may have seasonal allergies in school. The early skin symptoms were often the first sign of a broader allergic tendency.
For an evidence-based overview, the National Eczema Association explains how genetics and the skin barrier contribute to disease risk.
3. The Immune System Overreacts to Harmless Triggers
Another key part of how does eczema develop is immune dysregulation. In eczema, the immune system often reacts too strongly to things that are normally harmless, such as dust, pollen, fragrance, or certain fabrics.
This overreaction is often driven by Th2 immune pathways. These pathways release inflammatory cytokines, including interleukins such as IL-4 and IL-13. Those signals increase inflammation, itching, and barrier damage.
What this feels like
The skin may react as if it is under attack, even when the trigger is minor. A tiny amount of detergent residue or a shift in weather can set off redness and itching.
How inflammation harms the skin
- Increases itch intensity
- Causes swelling and redness
- Slows barrier repair
- Triggers the itch-scratch cycle
- Raises infection risk
The itch-scratch cycle is especially damaging. Scratching may bring a few seconds of relief. But it tears the skin surface and fuels more inflammation. Over time, the skin can become thick, darkened, and more sensitive.
Researchers at the National Institute of Arthritis and Musculoskeletal and Skin Diseases describe atopic dermatitis as a disease involving both barrier defects and immune system dysfunction.
4. Environmental Triggers Can Switch Eczema On or Make It Worse
Genes load the gun, but the environment often pulls the trigger. Many people notice that flare-ups start or worsen after specific exposures. This is why two people with similar genetics may have very different eczema experiences.
Common environmental triggers
- Dry air or sudden weather changes
- Dust mites
- Pollen
- Pet dander
- Air pollution
- Harsh soaps and detergents
- Fragranced skincare products
- Wool or rough fabrics
For some people, diet plays a role too. Spicy foods, oily meals, or specific allergens may worsen symptoms. This is not true for everyone, so it helps to track patterns carefully.
Lifestyle factors also matter
- Poor sleep
- High stress
- Frequent hot showers
- Overwashing
- Sweating without rinsing off
Stress is a major but overlooked trigger. A tense week at work or school can worsen itching, disturb sleep, and lower the skin’s ability to recover.
Quick trigger tracker
If flare-ups seem random, try recording:
- What you ate
- Weather changes
- New products used
- Stress level
- Hours of sleep
- Laundry detergent or fabric exposure
This simple habit often reveals patterns that were easy to miss.

5. The Skin Barrier Breaks Down, Leading to Dryness, Infection, and Chronic Damage
At the center of eczema is the skin barrier. Think of it as a brick wall. The skin cells are the bricks, and protective fats and proteins are the mortar. In eczema, the mortar becomes weak. Gaps form. Moisture escapes, and outside irritants slip in.
This barrier failure explains much of the damage eczema causes.
What happens when the barrier weakens
| Factor | What Happens | Effect on Skin Health |
|---|---|---|
| Water loss | Moisture escapes quickly | Dryness, flaking, tightness |
| Irritant entry | Soaps, dust, fragrance enter skin more easily | Burning, redness, stinging |
| Allergen exposure | Immune system reacts to harmless substances | More inflammation |
| Microbe overgrowth | Bacteria like Staphylococcus aureus can spread | Infection risk increases |
| Repeated scratching | Skin tears and thickens | Slower healing, chronic patches |
When the skin barrier fails, even normal daily life becomes harder. A warm shower may sting. A sweater may itch. Handwashing can leave the skin cracked.
Why infection is a concern
Broken eczema skin is more vulnerable to bacteria, viruses, and fungi. Signs of infection include:
- Yellow crusting
- Pus or fluid
- Increased pain
- Swelling
- Fever
- Suddenly worsening rash
These symptoms deserve prompt medical attention.
For broader public health guidance, the American Academy of Dermatology offers reliable information on eczema symptoms, triggers, and treatment.
6. Eczema Can Start at Any Age, but It Often Changes Form Over Time
Many people think eczema is only a childhood condition. That is not true. It often begins in infancy, but it can appear in teenagers, adults, and even older adults.
Common patterns by age
Infants
- Often appears on cheeks, face, or scalp
- Skin may look red, moist, or “weepy”
- Babies may rub against bedding because of itching
Children
- Common in elbow folds and behind knees
- Also seen on wrists and ankles
- Scratching often worsens at night
Adults
- Can appear anywhere on the body
- Hands, eyelids, neck, and flexural areas are common
- Skin may become very dry, thick, and long-lasting
This changing pattern can make eczema harder to recognize. An adult with persistent hand rash may think it is only irritation from soap. But eczema may be driving the problem beneath the surface.
Emotional and social impact
Eczema affects more than skin. It can disturb sleep, limit clothing choices, and create self-consciousness. Children may struggle in school from poor sleep. Adults may avoid social events because of visible patches.
That impact is real, and it should not be minimized.
7. New Research and Treatments Are Changing the Outlook
Modern research has improved our understanding of how does eczema develop. It is no longer seen as one simple rash. It is a complex disease involving genes, immune signals, microbes, and environment.
Updated insights for 2025–2026
- Around 31 million Americans live with eczema
- About 204 million people worldwide are affected
- The U.S. economic burden exceeds $5 billion annually
- Genome-wide studies continue to identify new susceptibility genes
- Precision medicine is becoming more realistic
One major advance is the rise of biologic therapies. Drugs like dupilumab target immune pathways such as IL-4 and IL-13. These treatments can reduce inflammation in moderate to severe eczema when basic measures are not enough.
What treatment usually includes
- Thick moisturizers to restore the barrier
- Gentle cleansers
- Trigger avoidance
- Topical corticosteroids or non-steroid creams
- Antihistamines in select cases
- Wet wrap therapy for severe flares
- Biologics or systemic treatment for advanced disease
The best plan depends on age, severity, and flare pattern. Self-treatment alone may not be enough when eczema is frequent, infected, or affecting daily life.

Practical Steps to Protect Skin Health
Understanding the cause is helpful, but daily care matters just as much. If you are trying to reduce flare-ups, these steps are often useful:
- Moisturize within minutes after bathing
- Use fragrance-free skincare and laundry products
- Keep showers short and lukewarm
- Wear soft, breathable fabrics
- Trim nails to reduce damage from scratching
- Manage stress with simple routines like walking or breathing exercises
- See a dermatologist if symptoms keep returning
These steps do not “cure” eczema, but they can reduce the burden and help the skin heal.
FAQs
1. What is the main cause of eczema?
There is no single cause. Eczema usually develops from genetics, immune overreaction, and environmental triggers acting together.
2. Can eczema develop in adulthood?
Yes. Although it often starts in childhood, eczema can first appear in adults at any age.
3. Is eczema contagious?
No. Eczema is not contagious and cannot spread from person to person.
4. Why does eczema itch so much?
Inflammation affects skin nerves and barrier function. Scratching then worsens the irritation, creating an ongoing itch cycle.
5. Can food cause eczema?
Food does not cause all eczema, but some foods can trigger flares in certain people, especially children with allergies.
6. When should I see a doctor for eczema?
See a doctor if the rash is painful, infected, widespread, disturbing sleep, or not improving with gentle skincare.
Conclusion
So, how does eczema develop? It develops through a layered process. Genetics weaken the skin barrier. The immune system overreacts. Environmental triggers add more stress. Together, these forces cause dryness, inflammation, itching, and repeated flare-ups that can damage skin health over time.
The good news is that understanding the process makes eczema easier to manage. Early care, trigger awareness, barrier repair, and medical treatment can all improve quality of life. If symptoms are persistent or severe, speak with a dermatologist. Support is available, and newer treatments are expanding options every year.
References
- National Eczema Association. Eczema overview and skin barrier information.
- National Institute of Arthritis and Musculoskeletal and Skin Diseases. Atopic dermatitis overview.
- American Academy of Dermatology. Eczema symptoms, causes, and treatment guidance.