7 Proven Ways to Prevent Proliferative Diabetic Retinopathy and Protect Your Vision
Living with diabetes means managing more than blood sugar. It also means protecting the tiny blood vessels in your eyes. Proliferative Diabetic Retinopathy is the most advanced stage of diabetic eye disease. It can develop quietly, often without pain or early warning signs. Yet it can lead to bleeding inside the eye, retinal detachment, and permanent vision loss if ignored.
That is the hard truth. The hopeful truth is this: many cases can be delayed, controlled, or even prevented from causing severe damage. The key is early action, steady diabetes care, and routine eye checks. If you have diabetes, these seven proven strategies can help protect your sight for the long term.
What Is Proliferative Diabetic Retinopathy?
Before prevention, it helps to understand the condition.
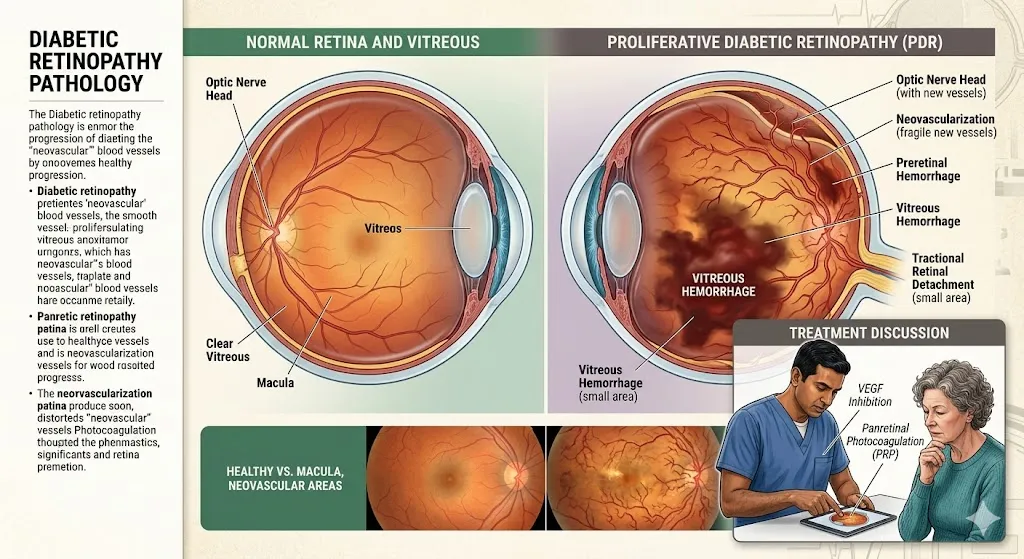
Proliferative diabetic retinopathy, or PDR, happens when diabetes damages the retina’s normal blood supply. The retina then becomes starved of oxygen. In response, the eye grows new blood vessels. These vessels are weak and abnormal. They can leak blood, create scar tissue, and pull on the retina.
This stage is dangerous because symptoms may appear late. A person may feel fine until vision suddenly becomes blurry or dark.
Common warning signs include:
- Floaters or dark spots
- Blurred or double vision
- Shadows in the field of vision
- Sudden loss of vision
- Eye pain or pressure in advanced cases
Still, many people have no symptoms at first. That is why prevention begins before you notice a problem.
1. Keep Blood Sugar in a Safe Range
High blood sugar is the main driver of diabetic retinal damage. Over time, excess glucose injures the small blood vessels that feed the retina. When circulation drops, the eye tries to compensate by growing fragile new vessels.
That is the exact process behind Proliferative Diabetic Retinopathy.
Why sugar control matters
The closer your glucose stays to your target range, the less stress your retinal vessels face. Consistent control matters more than occasional perfect readings.
Even modest improvements can reduce risk. Think of it like slowing rust on a bridge. You may not see the damage daily, but every day of protection counts.
Practical habits that help
- Check blood sugar as advised by your doctor
- Take insulin or medications on schedule
- Avoid long stretches of uncontrolled glucose
- Pair carbohydrates with protein or fiber
- Review your A1C regularly
A real-life example: someone with a high A1C for years may not notice eye damage early. But once glucose improves and follow-up eye care begins, progression often slows.
According to the National Eye Institute, controlling diabetes is one of the most effective ways to reduce diabetic eye complications.
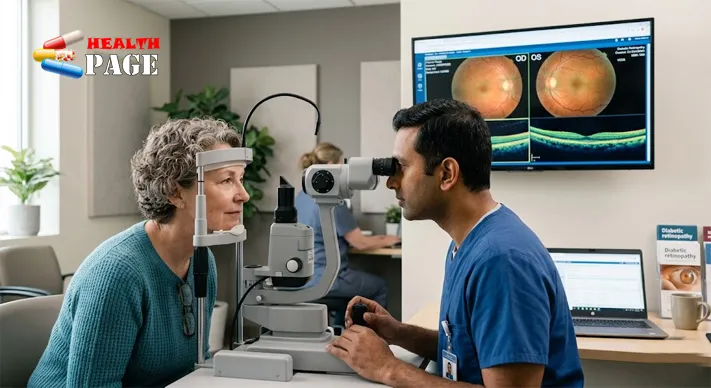
2. Never Skip Dilated Eye Exams
This is the most important prevention step.
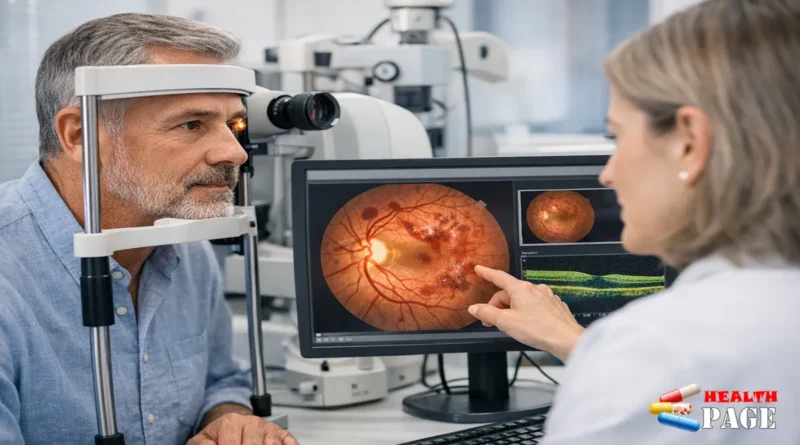
Early PDR often causes no pain and no obvious changes in sight. A standard vision test may also miss it. A dilated eye exam lets an eye specialist see the retina clearly and detect damage early.
Why early detection saves vision
When eye disease is found before bleeding or detachment begins, treatment works better. The goal is to act while vision is still stable.
A dilated exam can reveal:
- Retinal bleeding
- Swollen areas
- Abnormal new blood vessels
- Scar tissue
- Early macular changes
How often should you go?
Your schedule depends on your diabetes type, pregnancy status, and eye history. Many adults with diabetes need at least a yearly dilated exam. Some need more frequent visits.
People at higher risk include:
- Those with long-standing diabetes
- Pregnant women with diabetes
- People with kidney disease or nerve damage
- Patients with poor glucose control
If your retinal specialist recommends OCT, fluorescein angiography, or fundus photography, these tests can map changes in detail and guide treatment.
3. Control Blood Pressure and Cholesterol Too
Many people focus only on glucose. That is understandable, but incomplete. Eye health depends on the whole vascular system.
High blood pressure increases stress on already fragile blood vessels. High cholesterol can worsen circulation problems. Together, they raise the risk of retinal damage and vision-threatening complications.
The retina reflects your overall health
The eye is not separate from the rest of the body. It is like a window into your circulation. When blood pressure and cholesterol remain high, retinal tissue gets less support and more injury.
This is one reason experts now discuss diabetic retinopathy more broadly as diabetic retinal disease. Diabetes affects blood vessels, but also retinal nerve cells and support tissues.
What to discuss with your doctor
Ask about your:
- Blood pressure goal
- LDL cholesterol target
- Kidney function
- Medication adherence
- Lifestyle risk factors
A patient with diabetes, hypertension, and high cholesterol faces more than one source of retinal stress. Treating all three lowers the burden on the eyes.
The Centers for Disease Control and Prevention also stresses that managing blood pressure and diabetes together helps protect vision.
4. Act Fast on Early Symptoms
Many people wait too long because symptoms come and go. A few floaters may seem harmless. Slight blur may be blamed on fatigue. But with advanced diabetic eye disease, delay can be costly.
Symptoms that deserve urgent attention
Call an eye doctor promptly if you notice:
- Sudden floaters
- Flashing lights
- Dark curtain-like shadow
- Rapid vision blur
- Eye pain or pressure
These can signal bleeding, retinal traction, or even neovascular glaucoma.
Why timing matters
Abnormal vessels in PDR are brittle. They can bleed into the vitreous, the gel-like center of the eye. Scar tissue may then form and pull the retina out of place.
That shift can happen quickly. Early treatment often prevents a crisis.
A simple rule helps: if your vision changes suddenly, do not wait for your next routine appointment.
5. Understand the Treatments Before You Need Them
Prevention also means being informed. If your doctor finds severe diabetic retinal disease, knowing the options reduces fear and helps you act faster.
Modern treatment has improved a lot. Many people keep useful vision with timely care.
Main treatment options
| Treatment | What It Does | Best Use | Key Limitation |
|---|---|---|---|
| Panretinal Photocoagulation (PRP) | Uses laser to reduce signals that trigger new vessel growth | Long-term control of retinal neovascularization | May reduce peripheral or night vision |
| Anti-VEGF Injections | Blocks growth signals for abnormal vessels | Fast regression of new vessel growth and swelling | Needs repeat treatments |
| Vitrectomy Surgery | Removes blood and scar tissue from the eye | Non-clearing hemorrhage or traction retinal detachment | Surgery carries recovery time and risk |
Why combination care often works best
One treatment is not always enough. A patient may need anti-VEGF injections to shrink vessels quickly, followed by laser for longer control. If bleeding or traction becomes severe, surgery may be added.
That layered approach is often the strongest defense against blindness.
The American Academy of Ophthalmology provides trusted information on diabetic retinopathy treatment and eye exam timing.
6. Pay Attention to Pregnancy, Kidney Disease, and Diabetes Duration
Not all diabetes risk is equal. Some people need closer monitoring because their chances of progression are higher.
Longer diabetes duration raises risk
The longer you live with diabetes, the more time blood vessels have to accumulate damage. This is true for both type 1 and type 2 diabetes.
PDR is seen in a smaller share of all people with diabetes, but rates rise sharply in some younger insulin-dependent patients.
Pregnancy can speed progression
Pregnancy changes hormones, fluid balance, and circulation. In people with diabetes, those shifts can accelerate retinal changes. Eye checks before pregnancy and during pregnancy are especially important.
Kidney and nerve problems are warning flags
If diabetes is affecting your kidneys or nerves, your eyes may also be under strain. These complications often travel together because they share the same root problem: blood vessel damage.
Who should be extra careful?
You may need closer retinal monitoring if you have:
- Diabetes for many years
- Insulin dependence from a young age
- Pregnancy with diabetes
- Diabetic kidney disease
- Diabetic neuropathy
- A history of poor glucose control
This is where personalized care matters. Prevention is not one-size-fits-all.
7. Build a Long-Term Vision Protection Plan
The best prevention is not a single appointment. It is a system. It is the small, repeated choices that protect your sight year after year.
Your eye-health checklist
Create a plan that includes:
- Annual or specialist-recommended dilated eye exams
- A1C monitoring
- Blood pressure control
- Cholesterol management
- Medication adherence
- Smoking cessation if applicable
- Fast response to visual changes
Use tools that make follow-through easier
Try practical supports such as:
- Phone reminders for eye appointments
- Shared care notes between your diabetes doctor and eye doctor
- Family support for transport and follow-up
- Tele-ophthalmology screening where specialists are hard to reach
This matters even more in South Asia and other underserved regions. Many patients live far from retinal specialists. In those settings, screening programs and telemedicine can prevent late diagnosis.
Looking ahead: what is changing in 2025–2026?
Research is moving in a promising direction:
- Longer-acting anti-VEGF drugs may reduce injection frequency
- More personalized care may link retinal treatment with kidney and heart health
- New language such as diabetic retinal disease reflects a broader understanding of retinal injury
- Stem cell and retinal implant research continues, though it is not routine care yet
These advances are encouraging. But they do not replace early detection. They support it.
Why Awareness Still Matters
One major problem remains: many people with diabetes still do not know that serious retinal disease can develop silently.
They may seek help only after bleeding starts or vision drops. By then, treatment becomes more urgent and more complex.
This awareness gap affects quality of life in deep ways:
- Loss of driving ability
- Trouble reading medication labels
- Higher fall risk
- Loss of work independence
- Emotional stress and anxiety
Prevention is not only about preserving eyesight. It is about preserving confidence, mobility, and daily freedom.
If vision has already been affected, low-vision services, magnifiers, brighter lighting, and adaptive tools can still help people live well. That part of care is often overlooked, but it matters deeply.
FAQs About Proliferative Diabetic Retinopathy
1. Can proliferative diabetic retinopathy be reversed?
It can often be controlled, and abnormal vessels can regress with treatment. But damage from advanced bleeding or detachment may not fully reverse.
2. Does PDR always cause symptoms early?
No. Early Proliferative Diabetic Retinopathy may have no symptoms at all. That is why dilated eye exams are essential.
3. Is laser treatment still used if injections are available?
Yes. PRP laser remains a key treatment. Many patients do best with both laser and anti-VEGF therapy.
4. How quickly can PDR cause vision loss?
Sometimes gradually, sometimes suddenly. Bleeding or retinal traction can lead to rapid vision changes.
5. Can type 2 diabetes cause severe retinal disease too?
Yes. Both type 1 and type 2 diabetes can lead to proliferative diabetic eye disease, especially with long duration or poor control.
6. What is the best way to prevent it?
Control blood sugar, blood pressure, and cholesterol. Then keep every recommended dilated eye exam.
Conclusion
Proliferative Diabetic Retinopathy is serious, but it is not hopeless. In many cases, severe vision loss can be prevented with steady diabetes care and early eye monitoring. The seven steps are simple in principle: manage blood sugar, protect your blood vessels, watch for symptoms, and never skip retinal exams.
If you live with diabetes, do not wait for blurry vision to be your first signal. Schedule your eye check, review your numbers, and make vision protection part of your routine. Small actions today can help preserve your sight for years to come. 👁️
References
- National Eye Institute: diabetic retinopathy
- American Academy of Ophthalmology: diabetic retinopathy treatment