Lyme Disease ICD 10: 9 Powerful Tips for Correct Code Use, Chronic Cases, and History
If you work with medical records, you know how stressful it can be to choose the right Lyme disease ICD 10 code. Small coding mistakes can delay payment, create denials, or misrepresent a patient’s true condition.
Lyme disease itself is already complex. Symptoms can be vague, chronic issues can linger, and documentation is often incomplete. Add ICD-10 rules on top of that, and it is easy to feel overwhelmed.
This article walks you through practical, real-world tips to handle:
- The main Lyme disease ICD 10 code
- How to think about chronic Lyme disease ICD 10 coding
- The correct way to code history of Lyme disease ICD 10
- Common pitfalls and how to avoid them
Use this as an educational guide, not as a replacement for official instructions. Always cross-check with your organization’s policies and the ICD-10-CM Official Guidelines for Coding and Reporting for final decisions.
1. Start With the Basics: What Lyme Disease Is and Why Coding Matters 🧭
Before assigning any code, it helps to remember what you are coding.
Lyme disease is:
- A tick-borne infection caused by Borrelia bacteria
- Often transmitted by blacklegged ticks (deer ticks)
- Linked to symptoms like rash, fever, fatigue, joint pain, and neurologic issues
From a coding and clinical perspective, accurate diagnosis coding helps:
- Reflect the patient’s true condition on the record
- Support appropriate treatment and follow-up
- Ensure claims match documentation
- Enable tracking of disease patterns over time
A patient might present with:
- Early localized disease (erythema migrans rash)
- Early disseminated disease (neurologic or cardiac involvement)
- Late manifestations like arthritis or neuropathies
Your job as a coder or clinician is to translate that clinical picture into the right Lyme disease ICD 10 code or combination of codes.
Example: A patient with a classic bull’s-eye rash after a documented tick bite, treated with antibiotics, is different from a patient with long-term joint pain and unclear previous history. Your coding approach should recognize that difference.
2. Know the Core Lyme Disease ICD 10 Code (A69.2 Series) 🩺
The foundation of Lyme coding is the A69.2 category.
In ICD-10-CM, Lyme disease is coded primarily with:
- A69.20 – Lyme disease, unspecified
- A69.21 – Meningitis due to Lyme disease
- A69.22 – Other neurologic disorders in Lyme disease
- A69.23 – Arthritis due to Lyme disease
- A69.29 – Other conditions associated with Lyme disease
Many people casually refer to “the lyme disease icd 10 code” as if there is only one, but in practice, the A69.2x subcodes let you be more specific.
How to choose within A69.2x
- Use A69.20 when documentation states Lyme disease but does not specify a manifestation.
- Use a more specific code (like A69.23) when the provider clearly documents arthritis due to Lyme disease.
- Avoid guessing. If documentation is unclear, query the provider when possible.
Example: If the note says “Lyme arthritis of the right knee, confirmed by testing,” A69.23 (Arthritis due to Lyme disease) is usually more appropriate than A69.20.
A helpful habit is to read all A69.2x code descriptions in the manual or encoder. That way, you do not miss a more exact match.
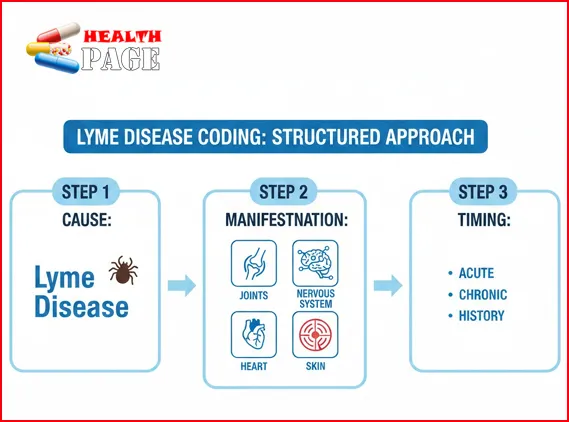
3. Use a Structured Approach: Symptom, Cause, and Timing 🧩
Lyme disease can show up in different ways:
- Skin (erythema migrans rash)
- Joints (arthritis)
- Nervous system (meningitis, neuropathy, cognitive issues)
- Heart (carditis)
To keep things consistent, think in three steps:
- Identify the confirmed or suspected cause
- Is Lyme disease documented as confirmed, probable, or suspected?
- Identify the primary manifestation
- Arthritis, meningitis, neuropathy, rash, etc.
- Identify timing or status
- Active infection, resolving, or long-term sequelae
This structure helps you decide:
- When to use A69.2x as the main diagnosis
- When to pair A69.2x with additional codes for manifestations
- When to code personal history instead of active disease
Example: A patient with “resolved Lyme disease, now with chronic neuropathic pain” may require coding for sequelae or residual symptoms rather than an active Lyme infection code.
4. Chronic Lyme Disease: Code the Reality, Not the Debate ⏳
“Chronic Lyme disease” is a sensitive and sometimes controversial term. Patients may use it to describe ongoing symptoms, while providers and guidelines may use other terminology.
From an ICD-10-CM standpoint, there is no single dedicated
chronic lyme disease icd 10 code.
Instead, your job is to:
- Identify whether there is active infection documented
- Determine whether the provider is describing sequelae (long-term consequences)
- Code the actual documented condition, not assumptions
Possible approaches (always depending on documentation):
- Use an A69.2x code if the provider documents current Lyme disease with active manifestations.
- Use codes for specific symptoms or sequelae (for example, neuropathy, arthralgia, fatigue) if Lyme is no longer active but caused lasting damage.
- If the provider documents “history of treated Lyme disease with current joint pain,” you may need a combination of:
- A personal history code
- A code for the current joint issue
Example: A patient seen for long-standing fatigue and joint pain after treated Lyme disease. Provider documents “no evidence of active infection, likely sequelae.” You would typically code the fatigue and joint symptoms and consider a personal history code rather than an active A69.2x code.
When in doubt, query the provider to clarify whether Lyme disease is current or historical.
5. History of Lyme Disease ICD 10: Don’t Mislabel Past as Present 📜
One of the most common errors is treating a past infection as if it were an active one. The ICD-10-CM has specific options for history of lyme disease icd 10 scenarios.
The key personal history code is:
- Z86.19 – Personal history of other infectious and parasitic diseases
You would generally use Z86.19 when:
- The patient had Lyme disease in the past
- The infection has been treated and resolved
- There are no current active signs of Lyme disease
- The historical infection is relevant to the current encounter
This is different from coding an acute episode:
- Do not use A69.2x solely for a past, treated disease with no active issues.
- Do use Z86.19 when the provider documents resolved Lyme disease, and this matters to the current care.
Example: A patient scheduled for surgery mentions treated Lyme disease 10 years ago, with no ongoing symptoms. Coding Z86.19 helps capture that history without implying active infection.
6. Combine Codes Wisely for Complex Presentations 🧠
In many charts, Lyme disease shows up alongside other problems. Coding often requires multiple codes to capture the full picture.
When to consider additional codes
- There is a specific organ complication (for example, meningitis, carditis).
- The provider documents systemic symptoms like fever or malaise.
- There are long-term consequences such as chronic pain or neuropathy.
You might see combinations like:
- A69.21 (Meningitis due to Lyme disease) as principal diagnosis
- Plus separate codes for symptoms or secondary conditions, if relevant and allowed
Or:
- A69.23 (Arthritis due to Lyme disease)
- Plus a code for a specific joint if documentation supports it, depending on your local rules
Always:
- Follow the ICD-10-CM Official Guidelines for Coding and Reporting
- Check any payer- or facility-specific instructions
- Avoid duplicating conditions with overlapping codes
Example: A chart documents “Lyme carditis causing conduction block.” You may need a Lyme disease code plus a code for the specific cardiac conduction disorder.
For deeper clinical background, reviewing trusted clinical references on Lyme disease such as the CDC page at Lyme disease can help you understand manifestations you see in documentation.
7. Use This Quick Reference Table for Common Lyme Coding Scenarios 📊
The table below summarizes frequent clinical situations and the typical code approaches. Always confirm with current guidelines and documentation.
| Clinical Scenario | Coding Approach (Example) | Notes |
|---|---|---|
| Active Lyme disease, no specific manifestation documented | A69.20 – Lyme disease, unspecified | Use when Lyme disease is confirmed but not otherwise specified. |
| Lyme meningitis | A69.21 – Meningitis due to Lyme disease | Principal code when meningitis is the main reason for encounter. |
| Lyme-related neurologic disorder (other than meningitis) | A69.22 – Other neurologic disorders in Lyme disease | Add additional neurologic codes if required. |
| Arthritis clearly documented as due to Lyme disease | A69.23 – Arthritis due to Lyme disease | Use when provider links arthritis directly to Lyme. |
| Other specified conditions associated with Lyme disease | A69.29 – Other conditions associated with Lyme disease | For documented Lyme-related conditions not covered elsewhere. |
| Past treated Lyme disease, no active signs | Z86.19 – Personal history of other infectious and parasitic diseases | Use when history is clinically relevant. |
| Persistent symptoms after treated Lyme disease, no active infection documented | Codes for symptoms (e.g., fatigue, pain) + Z86.19 | Consider sequelae; do not assume active infection without documentation. |
This is a reference aid, not a substitute for official manuals. Some encounters will need more codes than shown here.

8. Avoid Common Pitfalls With Lyme Disease ICD 10 Coding ⚠️
Even experienced coders get tripped up by Lyme disease. Here are some frequent issues and how to avoid them.
Pitfall 1: Coding Lyme without provider confirmation
Do not code Lyme disease solely based on:
- Patient self-report
- Prior history entries without clear current assessment
- Vague symptoms like “fatigue” or “joint pain”
You generally need provider documentation stating Lyme disease is suspected, probable, or confirmed, depending on your institution’s policies.
Pitfall 2: Confusing “history of Lyme” with active infection
As discussed, use Z86.19 for history without active disease. Do not code A69.2x unless documentation clearly indicates current infection or ongoing Lyme-related condition.
Pitfall 3: Forgetting to code the manifestation
If documentation states “arthritis due to Lyme disease,” do not stop at A69.20. Use the more specific A69.23 and add additional codes if guidance supports this.
Pitfall 4: Overusing the term “chronic Lyme”
Remember that ICD-10-CM does not provide a stand-alone
chronic lyme disease icd 10 code. Your coding should reflect:
- Active vs past infection
- Documented sequelae or residuals
- The exact wording used by the provider
Example: If a note only states “chronic Lyme” without detail, you may need to request clarification so that the code reflects a specific, documented condition.
9. Strengthen Your Workflow With Documentation and Education 📚
Accurate Lyme coding is not only about memorizing codes. It depends on strong documentation and ongoing education.
Encourage clear provider documentation
Ask providers to specify:
- Whether Lyme disease is active, suspected, or historical
- The main body system affected (joints, nervous system, heart, skin)
- Whether current symptoms are due to Lyme disease or another cause
- If long-term symptoms are sequelae of past Lyme disease
Simple documentation phrases like:
- “History of treated Lyme disease, no current infection”
- “Arthritis due to Lyme disease, active”
…can make coding far more accurate and defendable.
Keep resources handy
Maintain easy access to:
- The latest ICD-10-CM Official Guidelines for Coding and Reporting (available from CMS and other official sites)
- Internal coding policies for infectious diseases
- Clinical education on Lyme disease epidemiology and treatment patterns
Example: A quick, one-page internal reference sheet summarizing A69.2x and Z86.19, plus common scenarios, can save time and reduce denials.
Also, consider periodic reviews of infectious disease coding within your team, using anonymized real cases to practice consistent, compliant decisions.
FAQs About Lyme Disease Coding ❓
1. What is the main Lyme disease ICD 10 code?
In ICD-10-CM, the main category is A69.2 for Lyme disease. More specific subcodes like A69.20, A69.21, A69.22, A69.23, and A69.29 describe particular manifestations such as unspecified disease, meningitis, neurologic disorders, arthritis, and other conditions associated with Lyme.
2. Is there a specific chronic Lyme disease ICD 10 code?
There is no single, exclusive
chronic lyme disease icd 10 code. Instead, you code:
- The current documented condition (for example, arthritis due to Lyme disease)
- Any relevant symptoms or sequelae
- A personal history code, such as Z86.19, when Lyme disease is past and resolved
Always base your choice on provider documentation and official guidelines.
3. How do I code a history of Lyme disease ICD 10?
For a past, treated Lyme infection with no current active disease, use:
- Z86.19 – Personal history of other infectious and parasitic diseases
This captures the history of lyme disease icd 10 scenario when relevant to the encounter. Do not use A69.2x in this situation unless the provider documents active disease.
4. Should I code Lyme disease if only the patient mentions it?
Typically, you should not assign a Lyme disease code based only on patient report. You need documentation from the provider that:
- Confirms, suspects, or evaluates Lyme disease
- Or clearly states a relevant history
If the provider documents only symptoms, you code those symptoms according to your organization’s policies.
5. Where can I learn more about Lyme disease itself?
For clinical background and patient-focused information, reliable sources include public health agencies. One widely used reference is the CDC resource on Lyme disease, which explains transmission, symptoms, and treatment in more detail.
Conclusion: Bringing It All Together 👍
Accurate use of Lyme disease ICD 10 codes requires a blend of clinical understanding, careful reading of documentation, and familiarity with A69.2x and Z86.19. When you approach each chart methodically—distinguishing active disease, chronic manifestations, and history only—you protect both patients and your organization.
Remember to:
- Use the full A69.2x range, not just a single generic code
- Recognize that there is no dedicated “chronic Lyme disease” code
- Apply history of Lyme disease ICD 10 coding when infection is past and resolved
- Combine codes thoughtfully to reflect real-world complexity
By applying these nine tips consistently, you can code Lyme disease encounters with more confidence, reduce denials, and support accurate care documentation. If you feel unsure in a difficult case, pause, review the ICD-10-CM Official Guidelines for Coding and Reporting, and, when appropriate, request provider clarification. That extra step can make all the difference.


