Glimepiride: 7 Powerful Facts About Its Drug Class, Uses, and Side Effects
Managing type 2 diabetes can feel overwhelming, especially when you are prescribed new medications like glimepiride. Understanding what this drug does, how it works, and what to watch for can make you feel more in control of your health. This guide walks you through glimepiride in clear, practical language so you can partner confidently with your healthcare team. 💊
1. Glimepiride’s Drug Class: A Modern Sulfonylurea for Type 2 Diabetes
Glimepiride belongs to a group of medicines called sulfonylureas. These drugs have been used for decades to treat type 2 diabetes, but glimepiride is a more modern member of this class.
- Drug class: Second-generation sulfonylurea
- Sometimes labeled: “Third-generation” due to unique structural changes
- Approved by the FDA: 1995
- Primary indication: Type 2 diabetes in adults
You may see glimepiride sold under brand names like:
- Amaryl (widely used in the US)
- Duetact (glimepiride + pioglitazone)
- Tandemact (in some regions, also a combination product)
What is glimepiride used for?
Glimepiride is used for improving blood sugar control in adults with type 2 diabetes when diet and exercise alone are not enough. It can be prescribed as:
- Monotherapy (used alone)
- Combination therapy with:
- Metformin
- Insulin
- Thiazolidinediones (such as pioglitazone or rosiglitazone)
It is not helpful for type 1 diabetes, diabetic ketoacidosis, or for people whose pancreas produces very little or no insulin.

2. How Glimepiride Works: Stimulating Insulin Release and Improving Sensitivity
Understanding how glimepiride works can help you see why it lowers blood sugar effectively and why hypoglycemia is its main risk.
Primary mechanism: Triggering insulin release
Glimepiride acts directly on the pancreatic beta cells, which are the cells that make insulin. It does this by:
- Blocking ATP-sensitive potassium channels (KATP) on beta cells
- This causes cell depolarization (a change in electrical charge)
- Depolarization opens calcium channels, allowing calcium to flow into the cell
- The increase in calcium triggers exocytosis of insulin granules
- Result: More insulin is released into the bloodstream
This insulin release helps lower:
- Fasting blood glucose (before meals)
- Postprandial glucose (after meals)
- HbA1c (average blood sugar over 2–3 months)
Secondary effects: Helping the body use insulin better
Evidence suggests glimepiride may also:
- Increase peripheral tissue sensitivity to insulin
- Enhance glucose uptake into muscles and fat cells
This dual effect—more insulin and better use of that insulin—makes it a strong blood sugar–lowering medication.
How does it compare with other sulfonylureas?
Among sulfonylureas, glimepiride is often preferred for its balance of potency and safety:
- Longer duration of action than glipizide
- Lower risk of hypoglycemia and adverse cardiovascular effects than glyburide (glibenclamide)
For more detailed pharmacology, trusted sources like according to article/topic (e.g., a reputable pharmacology or diabetes reference site) provide in‑depth comparisons of sulfonylurea drugs.
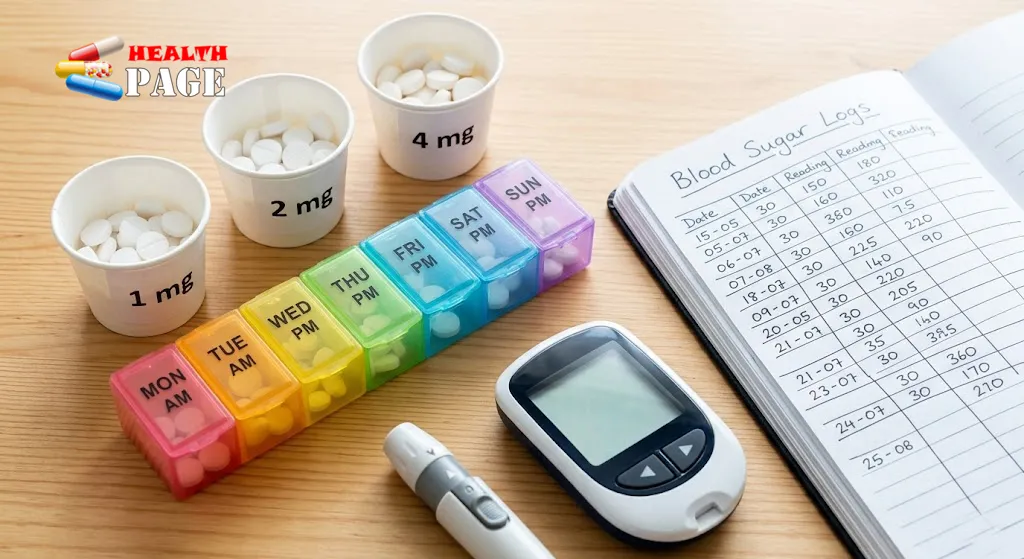
3. Dosage and Administration: From Glimepiride 2 mg to the Maximum Dose
Glimepiride is taken by mouth as a tablet. Your dose is tailored to your blood sugar levels, other medications, and overall health.
Common dosage forms
You’ll usually see strengths like:
- Glimepiride 1 mg
- Glimepiride 2 mg
- Glimepiride 4 mg
- Some markets also offer 6 mg and 8 mg tablets
Typical starting dose
For most adults:
- Start with 1–2 mg once daily
- Taken with breakfast or your first main meal
- Your provider may increase the dose every 1–2 weeks, depending on your blood sugar
Many people eventually reach:
- 4 mg once daily – this often provides near-maximal effect for many patients
- Maximum recommended dose is usually 8 mg/day
Your doctor will adjust slowly to reduce the risk of hypoglycemia. Never change your dose on your own without medical advice.
Special situations
- Older adults (elderly):
- More sensitive to hypoglycemia
- Doctors often start with 1 mg and adjust carefully
- Children:
- Safety and effectiveness not established
- Not routinely recommended in pediatric patients
- Kidney or liver problems:
- Dose adjustments may be needed
- More frequent monitoring is recommended
How to take glimepiride safely
- Take it at the same time each day
- Do not skip meals, especially breakfast, when you take the tablet
- If you miss a dose, take it when you remember unless it’s almost time for the next dose (never double up)
Example: Someone starts at glimepiride 2 mg, checks blood sugar regularly, and their doctor increases to glimepiride 4 mg when fasting levels remain high. Over a few weeks, their HbA1c improves with careful monitoring.
4. Pharmacokinetics: How Glimepiride Moves Through Your Body
Pharmacokinetics describes what your body does to the drug—how it is absorbed, distributed, metabolized, and eliminated.
Absorption
- Rapid and almost complete absorption from the gut
- Peak plasma concentration occurs about 2–3 hours after a dose
This is why taking glimepiride with your first main meal helps match its peak effect with rising blood sugar.
Protein binding
- Glimepiride is >99.5% bound to plasma proteins
- This means only a small free fraction is active, and it can potentially be affected by other highly protein-bound drugs
Metabolism
- Metabolized in the liver, mainly by the enzyme CYP2C9
- Converted into:
- M1 (active metabolite)
- M2 (inactive metabolite)
Changes in liver function or interactions with CYP2C9 inhibitors can increase glimepiride levels and side effect risk.
Elimination
- About 60% of metabolites are removed via the urine
- Around 40% via the feces
- Only a small amount of unchanged drug is excreted
Half-life
- Typical half-life is 5–8 hours
- With repeated dosing, it can extend up to about 9 hours
This half-life explains why once-daily dosing is usually enough. However, because its effect lasts many hours, missing meals or intense exercise without adjustment can trigger low blood sugar.
For a deeper look at diabetes medications’ pharmacokinetics, reputable resources like according to article/topic (for example, a recognized diabetes education site or guideline document) can help patients and clinicians compare options.
5. Glimepiride Side Effects: From Mild Symptoms to Serious Reactions
Like all medications, glimepiride carries side effects. Knowing what to look for helps you respond early and stay safe. ⚠️
Most common side effect: Hypoglycemia
Because glimepiride boosts insulin release, low blood sugar (hypoglycemia) is the main concern.
Typical symptoms include:
- Shakiness or tremor
- Anxiety or irritability
- Sweating, clammy skin
- Fast heartbeat
- Hunger
- Blurred vision
- Headache or dizziness
- Confusion or difficulty concentrating
If you feel these symptoms:
- Check your blood sugar if possible
- If low (usually under 70 mg/dL), treat with:
- 15 g of fast-acting carbs (e.g., 4 oz juice, glucose tablets, regular soda)
- Recheck in 15 minutes, repeat if still low
- Always follow your diabetes educator’s or doctor’s emergency plan
Other common glimepiride side effects
Some people notice:
- Mild nausea or stomach upset
- Headache
- Dizziness
- Slight weight gain (due to improved insulin action and calorie retention)
Often these symptoms improve over time as your body adjusts, but keep your provider informed.
Serious or rare side effects
Less common but more serious problems require urgent medical attention:
- Severe hypoglycemia
- Can cause seizures, loss of consciousness, or coma
- Emergency treatment with IV glucose or glucagon may be needed
- Allergic reactions (can be serious or life-threatening)
- Rash, itching, or hives
- Swelling of face, lips, tongue, or throat
- Trouble breathing or swallowing
- Hemolytic anemia (red blood cell breakdown), especially in people with G6PD deficiency
- Fatigue, pale skin, shortness of breath
- Dark urine, jaundice (yellowing of skin or eyes)
- Liver dysfunction
- Dark urine, pale stools
- Persistent nausea or vomiting
- Abdominal pain
- Yellow skin or eyes
If you suspect any serious reaction, stop the medication and seek urgent care.
Overdose
Taking too much glimepiride can cause prolonged and severe hypoglycemia. Signs include:
- Extreme weakness
- Confusion
- Loss of consciousness
- Seizure
Treatment usually involves:
- Oral glucose if the person is awake and able to swallow
- Intravenous glucose or glucagon injection in emergency settings
If you or someone nearby may have taken too much, call emergency services or poison control immediately.
6. Precautions, Contraindications, and Drug Interactions
Before starting glimepiride, your doctor will review your medical history and other medications. Some people should not use this drug, and others need closer monitoring.
Who should not take glimepiride?
Glimepiride is contraindicated (not recommended) in:
- Type 1 diabetes
- Diabetic ketoacidosis (DKA), with or without coma
- Known allergy to sulfonylureas or sulfonamide drugs
In these cases, insulin or other treatment approaches are necessary.
Use with caution in:
- Kidney disease (renal impairment)
- Risk of drug or metabolite build-up
- Higher chance of hypoglycemia
- Dose adjustment and frequent blood sugar checks are crucial
- Liver disease
- Metabolism may be reduced
- Increased risk of side effects
- Heart disease or cardiovascular risk
- While glimepiride may have a more favorable profile than glyburide, careful monitoring is still important
- G6PD deficiency
- Increased risk of hemolytic anemia
- Pregnancy and breastfeeding
- Limited human data
- Insulin is often preferred during pregnancy
- Discuss risks and benefits carefully with your obstetrician and endocrinologist
Always tell your healthcare team about your full medical history before starting glimepiride.
Key drug interactions
Glimepiride can interact with many common drugs. Some increase the risk of low blood sugar, while others reduce its effectiveness.
Drugs that may increase risk of hypoglycemia
- Insulin and other oral antidiabetic drugs
- Beta‑blockers (e.g., metoprolol, atenolol)
- They can also mask symptoms of low blood sugar such as rapid heartbeat
- Alcohol (especially binge drinking or drinking on an empty stomach)
Drugs that may reduce glimepiride’s effect
- Corticosteroids (e.g., prednisone)
- Thiazide diuretics (e.g., hydrochlorothiazide)
- Thyroid hormones (e.g., levothyroxine)
These can raise blood sugar and may require dose adjustments.
CYP2C9 inhibitors
Medications like fluconazole (an antifungal) can inhibit CYP2C9, the enzyme that metabolizes glimepiride. This can lead to:
- Higher glimepiride blood levels
- Greater risk of hypoglycemia
If you start or stop any major medication, always inform your prescriber so they can reassess your glimepiride dose.
7. Clinical Efficacy: How Well Does Glimepiride Work?
Glimepiride has been widely studied and used around the world. Clinical trials and real-world data show it is effective for many people with type 2 diabetes.
Blood sugar improvements
In controlled trials, glimepiride has been shown to reduce:
- Fasting plasma glucose by about 46 mg/dL
- Postprandial (after-meal) glucose by about 72 mg/dL
- HbA1c by roughly 1.4 percentage points compared with placebo
These changes can significantly reduce the risk of complications when combined with lifestyle changes.
Why glimepiride 4 mg is often a “sweet spot”
Many patients achieve near‑maximal benefit at glimepiride 4 mg daily. Higher doses (up to 8 mg) may not add much extra glucose lowering but can increase side effects.
Your provider will individualize your dose to achieve:
- Good blood sugar control
- Minimal hypoglycemia
- Acceptable side effects
How glimepiride compares with other options
Glimepiride is often chosen because it is:
- Cost-effective (often more affordable than some newer agents)
- Available in many countries
- Well understood by clinicians
However, newer drug classes (like SGLT2 inhibitors and GLP‑1 receptor agonists) may:
- Offer heart and kidney benefits
- Carry lower risk of hypoglycemia
- Support weight loss instead of weight gain
Your treatment plan might include glimepiride alone, or together with other drugs like metformin or SGLT2 inhibitors, depending on your overall health, financial considerations, and treatment goals.
Quick Comparison Table for Glimepiride
| Feature | Details |
|---|---|
| Drug class | Sulfonylurea (2nd generation) |
| Indication | Type 2 diabetes mellitus in adults |
| Max dose | 8 mg/day |
| Usual effective dose | Often 4 mg/day for near-maximal effect |
| Half-life | 5–8 hours (up to 9 hours with repeated dosing) |
| Protein binding | >99.5% |
| Metabolism | Hepatic via CYP2C9 → M1 (active), M2 (inactive) |
| Elimination | ~60% urine, ~40% feces (mostly metabolites) |
| Main risk | Hypoglycemia (low blood sugar) |
| Contraindications | Type 1 DM, diabetic ketoacidosis, sulfonamide allergy |
| Special caution | Elderly, renal impairment, G6PD deficiency, pregnancy, liver disease |
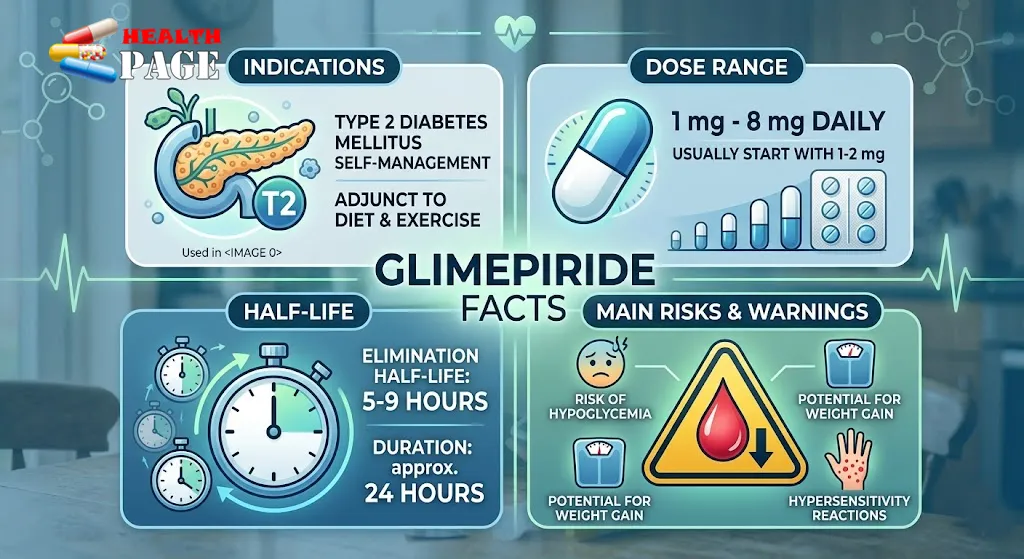
FAQs About Glimepiride
1. Is glimepiride insulin?
No. Glimepiride is not insulin. It is an oral medication that stimulates your pancreas to release more of your own insulin. Insulin itself is usually injected.
2. Can I take glimepiride with metformin?
Yes. Glimepiride is often combined with metformin to improve blood sugar control. The drugs work in different ways: metformin reduces liver glucose production and improves sensitivity, while glimepiride increases insulin release. Your doctor will adjust doses to minimize hypoglycemia.
3. Will glimepiride cause weight gain?
Mild weight gain can occur, as seen with many sulfonylureas, due to increased insulin action and improved calorie use. Healthy eating and regular physical activity can help limit this effect.
4. Is glimepiride safe for long-term use?
Glimepiride has been used for many years and is generally safe for long-term use when:
- Doses are appropriate
- Blood sugar and HbA1c are monitored
- Kidney and liver function are reviewed periodically
However, your doctor may adjust or change medications over time as your health or guidelines evolve.
5. Can I drink alcohol while taking glimepiride?
Alcohol can increase the risk of hypoglycemia, especially if you drink on an empty stomach or in large amounts. If you drink, do so in moderation, always with food, and monitor your blood sugar closely. Discuss your drinking habits honestly with your healthcare provider.
6. What should I do if I keep having low blood sugars on glimepiride?
Frequent lows are a warning sign. Contact your provider to review:
- Your current dose (e.g., glimepiride 2 mg vs glimepiride 4 mg)
- Meal timing and content
- Exercise schedule
- Other medications
A dose reduction, schedule change, or switch to another drug may be needed.
Conclusion: Using Glimepiride Wisely for Better Blood Sugar Control
Glimepiride is a well‑known, cost‑effective medication for type 2 diabetes. As a modern sulfonylurea, it lowers fasting and after‑meal glucose and improves HbA1c by stimulating insulin release and supporting better insulin use in the body. Many adults do well on doses like glimepiride 2 mg or glimepiride 4 mg once daily, often alongside metformin or other agents.
At the same time, this drug’s main risk—hypoglycemia—means that careful monitoring, regular meals, and open communication with your healthcare team are essential. People with kidney disease, liver problems, G6PD deficiency, or those who are pregnant or breastfeeding need individualized evaluation before starting treatment.
If you are taking or considering glimepiride:
- Discuss your full medical history and medications with your clinician
- Learn the signs of low blood sugar and how to treat it
- Keep regular follow‑ups to track HbA1c, kidney, and liver health
Used thoughtfully, glimepiride can be an important part of a broader plan that includes healthy eating, physical activity, and ongoing support—helping you live well with type 2 diabetes. 🌱
Note: This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance.
Dr. Sana Lodhi is a qualified medical doctor (MBBS) with a strong commitment to patient care and evidence‑based medicine. With years of clinical experience, she brings trusted medical insights to readers, simplifying complex health topics into clear, practical guidance. Her passion lies in promoting preventive healthcare, empowering individuals to make informed decisions, and bridging the gap between medical knowledge and everyday wellness. At HealthyPost.co.uk, Dr. Lodhi shares expert perspectives on health, lifestyle, and medical awareness to help readers live healthier, more balanced lives.


